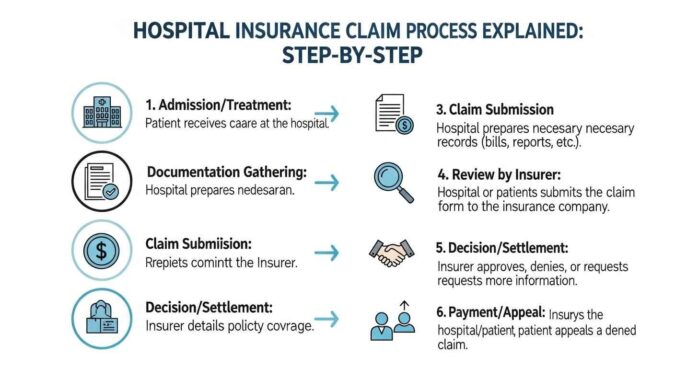
Learn the hospital insurance claim process explained, step-by-step guide for cashless and reimbursement claims with required documents and timelines.
How Cashless Hospital Claims Work
A cashless claim allows the insurance provider to pay the hospital directly for approved medical expenses. In the hospital insurance claim process explained, this option works only at a network hospital listed by the insurer.
After admission, the hospital’s insurance desk submits a pre authorization form to the third-party administrator (TPA) or insurer. The insurer reviews the policy details, coverage limits, and treatment information. Once approved, the hospital proceeds with treatment while billing is handled directly with the insurer.
The policyholder usually pays only non-covered costs such as deductible amounts, co-payments, or services outside policy coverage. This process reduces upfront financial pressure and simplifies hospital billing.
Expected Timelines for Hospital Insurance Claims
A reimbursement claim requires the policyholder to pay hospital expenses first and then request repayment from the insurer. In the hospital insurance claim process explained, this method is common when treatment occurs at a non-network hospital.
After discharge, the policyholder submits a claim form, itemized hospital bills, discharge summary, prescriptions, and diagnostic reports to the insurance provider or third-party administrator (TPA). The insurer reviews the documents, checks policy terms like sum insured, deductibles, and policy exclusions, and verifies the medical treatment.
Once verification is complete, the approved amount is transferred to the policyholder’s bank account as part of the claim settlement process.
| Step | Details |
|---|---|
| Definition | A reimbursement claim requires the policyholder to pay hospital expenses first and then request repayment from the insurance provider. Common for non-network hospitals. |
| Document Submission | After discharge, submit claim form, itemized hospital bills, discharge summary, prescriptions, and diagnostic reports to the TPA or insurer. |
| Insurer Review | The insurer checks policy terms, including sum insured, deductibles, policy exclusions, and verifies the medical treatment. |
| Settlement | Once verified, the approved amount is transferred to the policyholder’s bank account as part of the claim settlement process. |
| Purpose / Benefit | Ensures reimbursement for covered expenses while maintaining policy compliance and proper documentation. |
Required Documents Checklist
Submit all essential documents to ensure a smooth claim process. For the hospital insurance claim process explained, accurate and complete paperwork is critical for both cashless and reimbursement claims.
Key documents include the claim form, policy or ID proof, discharge summary, itemized hospital bills, prescriptions, and diagnostic reports. For reimbursement claims, also include bank account details for settlement. Missing or incorrect documents can delay approval or lead to rejection.
Organizing all paperwork beforehand helps the insurance provider or third-party administrator (TPA) process the claim efficiently and avoid unnecessary follow-ups.
Post-Submission: Verification & Settlement
After submitting your claim, the insurer verifies documents before approval. In the hospital insurance claim process explained, this step ensures that all treatment costs comply with the policy’s coverage, sum insured, and policy exclusions.
The insurance provider or third-party administrator (TPA) may request additional information or clarifications. Once verification is complete, approved amounts are settled either directly with the hospital (cashless) or transferred to the policyholder’s bank account (reimbursement).
Prompt and accurate submission of documents helps speed up the claim settlement process and reduces the risk of delays or rejections.
Common Claim Mistakes & How to Avoid Them
Many hospital insurance claims are delayed or rejected due to simple mistakes. In the hospital insurance claim process explained, common errors include late claim intimation, missing or incorrect documents, exceeding room rent limits, and misunderstanding cashless claim rules.
Other frequent issues involve billing errors or submitting claims to a non-network hospital without prior approval. Paying attention to policy terms like deductible amounts, co-payment clauses, and policy exclusions can prevent unnecessary complications.
Following proper procedures and double-checking all submissions ensures a smoother claim settlement process and increases the likelihood of timely approval.
Realistic Timelines & Expectations
Understanding typical claim timelines helps set realistic expectations. In the hospital insurance claim process explained, cashless claims at network hospitals are usually approved within a few hours, while reimbursement claims can take 10–30 days depending on document accuracy and insurer verification.
Delays may occur if additional information is requested or if there are discrepancies in discharge summaries, itemized bills, or other required documents. Knowing these timelines allows the policyholder to track progress effectively and follow up with the insurance provider or third-party administrator (TPA) without confusion.
Tips for Faster Settlements
Following simple steps can speed up your insurance claim. In the hospital insurance claim process explained, organize all required documents, including the claim form, discharge summary, prescriptions, and itemized hospital bills, before submission.
Always notify the insurance provider or third-party administrator (TPA) immediately after hospitalization and use the digital claim portal if available. Keep track of the claim reference number and follow up regularly to avoid unnecessary delays. Proper preparation and timely communication ensure a smoother and faster claim settlement process.
Steps to Take When a Hospital Claim Is Rejected
If your hospital insurance claim is rejected, there are clear steps to follow. In the hospital insurance claim process explained, first review the rejection reason carefully. Common causes include missing documents, delayed claim intimation, or treatment outside network hospital coverage.
You can resubmit the claim with complete documents or file an internal appeal with the insurance provider or third-party administrator (TPA). If the issue persists, approach the insurance ombudsman or grievance redressal forum. Taking prompt action increases the chances of overturning the rejection and securing your claim settlement.
FAQs – Hospital Insurance Claim Process Explained
Q1: What is the difference between cashless and reimbursement claims?
A1: Cashless claims are paid directly to the hospital by the insurer, while reimbursement claims require the policyholder to pay first and claim repayment later.
Q2: How long does a hospital insurance claim take?
A2: Cashless claims usually process within hours; reimbursement claims take 10–30 days depending on document completeness and verification.
Q3: What documents are required for a hospital insurance claim?
A3: Claim form, policy/ID proof, discharge summary, itemized hospital bills, prescriptions, diagnostic reports, and bank details.
Q4: Can my claim be rejected?
A4: Common reasons include late intimation, missing documents, exceeding policy limits, or treatment at a non-network hospital.